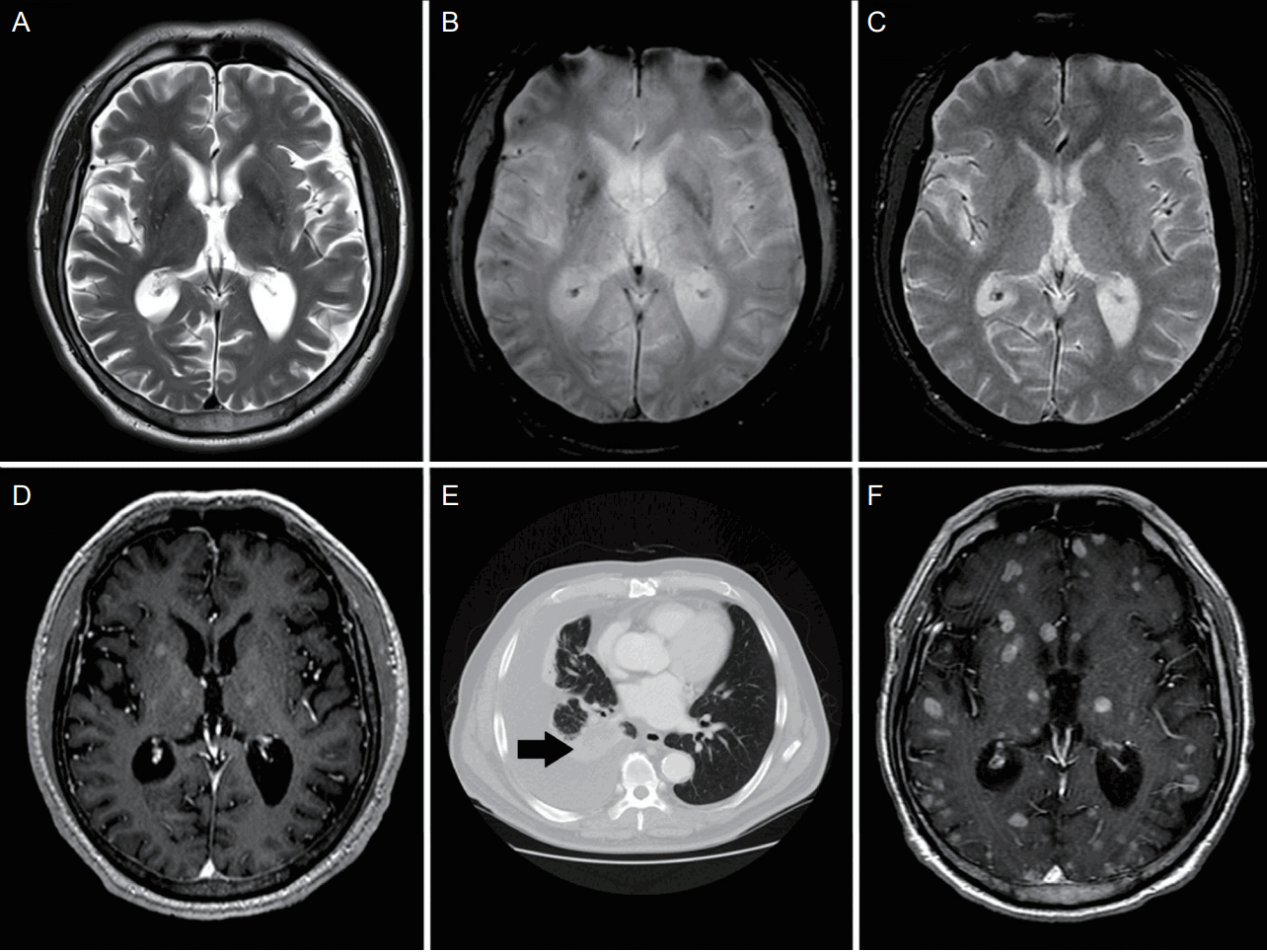
A 65-year-old man with hypertension and diabetes presented with a history of speech disturbance and gait disturbance of several months duration. He had a 50 pack-year smoking history. Neurologic examination revealed dysarthria and truncal ataxia. Initial vital signs and routine laboratory tests were unremarkable. Although the axial fluid attenuated inversion recovery, T1 and T2-weighted brain magnetic resonance imaging (MRI) revealed no definite evidence of abnormality (Fig. 1A), the T2-weighted gradient echo (GRE) images revealed multiple, hypo-intense lesions in the cortical and subcortical areas (Fig. 1B). In view of the particular patientŌĆÖs multiple risk factors for stroke, the presence of asymptomatic cerebral microbleeds were highly suspected. There were, however no findings to suggest microbleeds on a brain MRI, conducted 8 months earlier to evaluate a postural hand tremor (Fig. 1C).
Therefore, newly developed multiple microbleeds raised a suspicion of hemorrhagic brain metastasis, leading to a focus on finding, identifying and evaluating a potentially hidden malignancy. An additional, contrast-enhanced brain MRI revealed multiple, enhanced, nodular lesions (Fig. 1D). A chest computed tomography revealed a tumor in the lower lobe of the right lung with pleural effusion and multiple metastatic lymph nodes (Fig. 1E). A bronchoscopic lung biopsy was conducted and subsequently, poorly-differentiated adenocarcinoma was diagnosed. Two months after the initial diagnosis, the patient returned with report of a severe headache and nausea. A follow-up MRI revealed prominent multifocal enhancing nodules suggestive of progression of metastasis (Fig. 1F).
Metastases that are characterized by hemorrhage as (one) classic clinical sign include malignancies such as melanoma, choriocarcinoma, renal cell carcinoma, thyroid, lung and breast cancer. Of all hemorrhagic metastases, however, lung and breast cancers are the most common etiologies due to their higher overall prevalence [1]. Previous studies have demonstrated that hemorrhagic metastasis contain significantly higher levels of vascular endothelial growth factor (VEGF) and matrix metalloproteinases (MMP), when these malignancies were compared with non-hemorrhagic tumors [2,3]. The over-expressed VEGF and MMP increase the permeability of the blood vessels, resulting in microhemorrhages. In case of metastatic melanoma (that can appear hypointense on GRE),┬Āthe specific malignancy can often be distinguished from cerebral microbleed by the concomitant presence of T1 hyperintensity (caused by the melanin). However, it is difficult to differentiate between cerebral microbleed and hemorrhagic metastasis due to other primary cancers.
If there is no history of cancer or contrast-enhanced MRI, it can be challenging to differentiate hemorrhagic metastasis from cerebral microbleeds [4]. Detection by contrast enhanced methods may depend on the ratio of tumor vascularity to size. However, detection by T2-weighted gradientecho MRI depends on magnetic susceptibility. Thus, T2-weignted GRE MRI can detect much smaller hemorrhagic metastases than the smallest tumor that can be detected on contrast-enhanced MRI [5,6]. In addition, because there is a relatively restricted number of kinds of primary cancers that cause hemorrhagic metastases, GRE can enable identification of the primary cancer. Therefore, it is necessary to conduct brain MRI scans to include various sequences including GRE in to diagnose small hemorrhagic metastasis that may be undetected on T1-enhanced images.