INTRODUCTION
Neurogenic pulmonary edema (NPE) is the condition of non-cardiogenic abnormal accumulation of extravascular liquid in lungs due to acute central nervous system (CNS) injury [1]. Although epileptic seizure, cerebral hemorrhage, meningitis and traumatic brain injury are known to be the major contributors, NPE cases after cerebral infarction are relatively rare [2,3]. Herein, we described an acute middle cerebral artery infarction patient who experienced respiration difficulty requiring intubation and mechanical ventilation due to NPE.
CASE REPORT
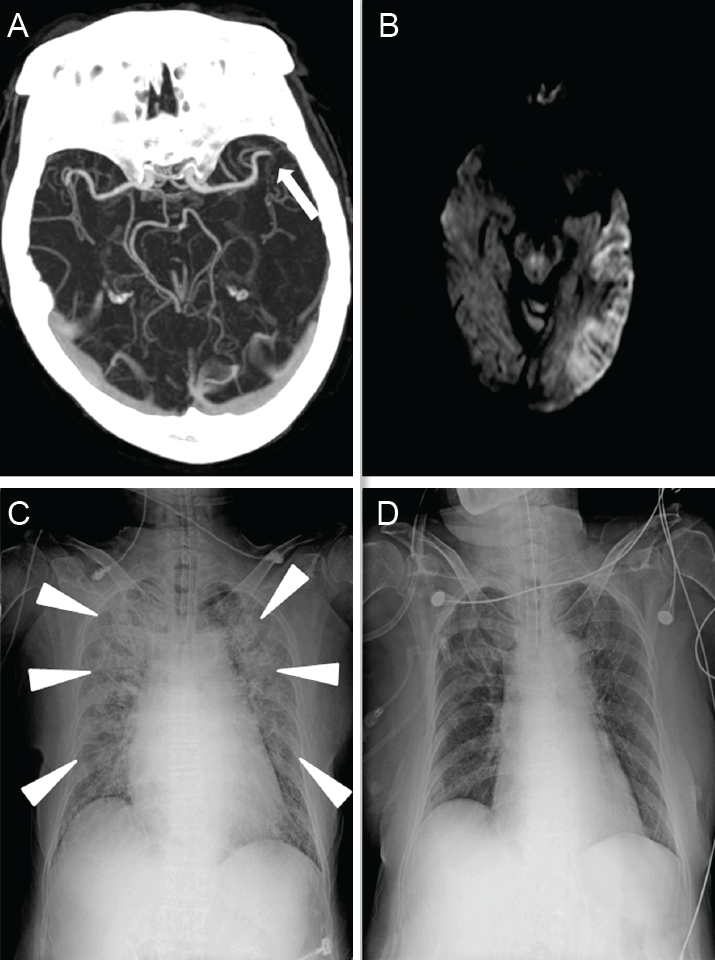
A 77-year-old Korean woman visited emergency room complaining of sudden onset right side weakness which started one hour ago. She had been previously diagnosed as lone atrial fibrillation with normal heart rate. Initial blood pressure was measured as 190/100 mmHg, pulse rate of 100 beats/min, body temperature of 36.8℃, normal respiratory rate with clear lung sound. Neurological examination revealed motor aphasia and right side weakness, with total National Institute Health Stroke Scale of 15. Brain computerized tomography angiography followed by brain magnetic resonance imaging showed left middle cerebral artery occlusion with acute cerebral infarction (Fig. 1A, B). Her laboratory study results were unremarkable.
Intravenous thrombolytic therapy was considered, but suspended because she suddenly complained of difficulty in breathing. Lung auscultation disclosed new rale from whole lung field with lip cyanosis. Jugular venous distention was absent. The oxygen saturation from oximeter monitoring decreased below 85%, necessitating emergent intubation. Arterial blood gas analysis after successful intubation showed elevated carbon dioxide level of 65.7 mmHg (normal range: 32-48 mmHg), slightly decreased bicarbonate of 21.4 mmol/L (normal: 22-31 mmol/L), and low pH with 7.14 (7.35-7.45), suggesting acute respiratory acidosis. The serum levels of cardiac enzyme, brain natriuretic peptide and D-dimer were normal. Followed chest radiography revealed bilateral interstitial infiltrate (Fig. 1C). Thrombolytic treatment with recombinant tissue plasminogen activator (0.9 mg/kg) was initiated after intubation, and she was transferred to intensive care unit and maintained with mechanical ventilation and intermittent diuretics. Portable echocardiography revealed normal cardiac function without wall motion abnormality. Her respiratory status was rapidly stabilized, and she was weaned from the ventilator on the 4th days after stroke onset (Fig. 1D).
DISCUSSION
This case describes NPE after acute cerebral infarction due to left middle cerebral artery occlusion, which showed favorable clinical course after intravenous thrombolysis treatment.
The pathophysiology of pulmonary edema following acute brain injury harbors massive adrenergic excitation-induced myocardial dysfunction, altered systemic/pulmonary hemodynamics by sympathetic surge, and pulmonary endothelial integrity disruption [2]. The possible mechanisms of NPE after cerebral infarction includes abrupt increase of intracranial pressure by large infarction or direct destruction of so called “NPE trigger zones” including insular cortex, hypothalamus or ventrolateral medulla [3,4]. Sudden disruption of blood supply toward left insular cortex after middle cerebral artery occlusion could be suggested as a possible etiology of NPE in this case. Rapid recovery after successful recanalization by intravenous thrombolysis supports this hypothesis. There has been a previous report describing NPE after left hemispheric infarction involving insular cortex, which was associated with cardiac dysfunction, but rapidly resolved after thrombolytic treatment [4]. Previous case control study describing pulmonary edema after cerebral infarction showed that brainstem infarction could result in isolated pulmonary edema, whereas suptratentorial hemispheric infarction involving insular cortex showed pulmonary edema with myocardial dysfunction, namely, “stunned myocardium [3]”.
The treatment principal of NPE includes rapid control of the triggering central nervous system insult and supportive treatment. The clinicians should consider NPE as one of the possible etiologies of sudden respiratory compromise after acute cerebral infarction, when other discernable causes had been excluded. Successful recanalization treatment could result in early improvement of pulmonary edema after acute cerebral infarction.